Having an allergy means that your body is sensitive to a substance that to most people is harmless. The substance causing the symptoms is called an allergen. Because the offending allergen is usually a specific protein, people may be allergic to only one substance, or to several.
The most common types of allergies are:
- Outdoor allergies
- Indoor allergies
- Animal allergies
- Insect allergies
- Medication allergies
- Food allergies
- Latex allergy
Important: You could be allergic to something not listed here. If you suspect you have an allergy, see the article “Do I have an Allergy?”, and be sure to discuss the symptoms with your doctor or other health care professional. According to the American Medical Association, about 40 million to 50 million Americans are affected by allergies.
1. Outdoor Allergies

Pollen. Trees, grasses and weeds reproduce by forming a fine, powdery substance called pollen. Air carries the pollen from the male structures to the female ones. Because it is airborne, pollen can enter the human body in several ways. As air is breathed in through the nose, nasal structures filter out the pollen. In the nasal mucus membranes the pollen comes into contact with the mast cells. Recognizing the pollen as an allergen, mast cells start producing histamine. The histamine dilates the blood vessels, causing swelling, inflammation and congestion. Because pollen is so fine, it can come in contact with the mucus membranes of the eyes, leading to watery, itchy eyes. Pollen that lands on hair, clothing or pet fur is touched by the allergy sufferer’s hands, which then touch the eyes or nose, creating the cascade of symptoms.
Most pollen allergies are respiratory, affecting the nose, eyes and mouth, making breathing difficult. They are usually seasonal. In certain climates, however, allergy sufferers may have little respite, especially if they are allergic to different pollens, which “bloom” throughout the year. Humidity usually makes the symptoms worse, as the pollen get trapped in the moisture of the air and remains airborne for longer periods of time.
Allergic rhinitis or hay fever. This type is an allergic reaction characterized by sneezing, coughing, itchy nose, mouth and throat, congestion and/or runny nose. The offending allergens are usually pollens, molds, dust mites and animal allergens. According to the Centers for Disease Control and Prevention (CDC), approximately 35 million Americans suffer from hay fever each year, with most sufferers being 45 or younger. Statistics indicate that close to 20 percent of the population in the United States suffers from allergic rhinitis. This adds up to $4 billion in lost work productivity! Allergic rhinitis is linked to chronic sinusitis, an inflammation of the facial sinuses, affecting some 35 million Americans. The National Institutes of Health’s Office of Alternative Medicine is studying the use of complementary therapies, including oral immunotherapy, for hay fever and other allergies.
2. Indoor allergies (molds and mites)
While pollen is more seasonal in nature, allergies to these indoor allergens run year-round, sometimes referred to as “perennial” (versus “seasonal”). Symptoms tend to be primarily respiratory in nature. Perhaps you only have problems when cleaning out a closet, or when spending long periods of time in a damp basement, or when cleaning the bathroom. Molds can be found both indoors as well as outdoors. Raking leaves or turning a mulch pile can be particularly irritating. Using a filter mask when performing these activities can lessen their negative effects. Dust mites are especially problematic, as the irritating particles are minute.. The treatment section discusses ways to minimize exposure. They particularly invade our beds.
3. Animal allergies (pets)

We love our pets; so allergies to our animals can be emotional. The allergen is not the hair or fur, but the dander. Whether the animal is housed outdoors, such as a horse or rabbit, or indoors, such as a cat or dog, the resulting allergic reaction is the same. With outdoor animals it is easier to limit the frequency and duration of exposure than with indoor pets. Certainly avoid having the pet in the bedroom. Of all the rooms in the house, the bedroom is the most important one to keep as clean of the allergen as possible. For most people the term pet is synonymous with “warm and fuzzy,” which includes anything with hair, fur or feathers. This leaves turtles, hermit crabs, and reptiles!
4. Insect Allergies
Insect bites and stings can be annoying, painful and localized, or can lead to a systemic allergic reaction known as anaphylaxis, a life-threatening medical emergency. A local reaction may include swelling of a whole arm or leg. This is not an allergic reaction, just a severe local reaction. Anyone who has experienced more than a local reaction to an insect bite or sting, such as swelling beyond the local area (fingers, arms, etc.), itching all over the body or any difficulty breathing, should discuss with their physician the prescription of an emergency epinephrine kit. Such a kit should be with the person at all times (see anaphylaxis). Wearing shoes, long pants and sleeves, and avoiding perfumes or scented deodorants can decrease exposure. For local redness, pain or swelling, a cool compress can minimize discomfort. Seek medical attention if symptoms go beyond the local site.
The Journal of the American Medical Association (JAMA) reported that up to 5 percent of the U.S. population experiences anaphylaxis due to insect stings, resulting in 40 deaths yearly.
5. Medication allergies
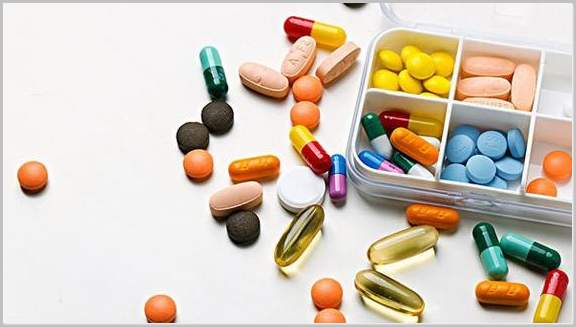
While any medication could potentially cause an allergic reaction, the drugs most likely to cause a reaction are: the antibiotics penicillin and tetracycline, sulfonamides (or “sulfa” drugs), antimicrobials used in the treatment of urinary tract infections, and local anesthetics in the “caine” family, such as novocaine and lidocaine.
Signs indicative of an allergic reaction to a drug include fever, hives (also called urticaria), itchy nose, throat or ears, and flushed skin. Symptoms of a stronger reaction may include coughing, swelling (“angioedema”), especially of the eyes or tongue, and cyanosis, a bluish tint of the skin.
You might notice flushed cheeks, and then with another dose find the redness has spread to your neck and is itchy. Call your doctor as soon as you suspect an allergic reaction. Each dose increases the risk of a stronger reaction, including the life-threatening anaphylaxis. Prevention is avoidance of the medication. Make sure any physician you see knows of your previous drug reaction.
To ease mild rash-like symptoms:
- Press on the area instead of scratching. Scratching increases inflammation and itching.
- Keep cool; overheating increases itching.
- A cool compress decreases discomfort.
- Find a distraction, such as listening to music, or doing something you enjoy. It helps to decrease awareness of the discomfort.
6. Food Allergies
While many people have adverse reactions to certain foods, less than 2 percent of adults and 5 percent of children suffer from a true food allergy. A food “intolerance” (which is not an immune response) may result in gastrointestinal symptoms such as the bloating, pain, cramping, and diarrhea associated with lactose intolerance. Lactase (an enzyme that helps you digest lactose) drops and tablets can substantially reduce the unpleasant symptoms. A true food allergy involves an allergic reaction, and is most often a reaction to the protein found in such foods as cow’s milk, egg whites, peanuts, shellfish and other seafood, tree nuts, wheat and soy. The reaction can occur right away, within a few hours, or even can be uncommonly delayed.
Symptoms of a food allergy can be:
- A skin reaction — such as rashes, hives or eczema
- Gastrointestinal — cramping, nausea, vomiting or diarrhea
- Respiratory — sneezing or runny nose, coughing, wheezing or shortness of breath. Other reactions can be subtle, such as itching in the mouth or throat and can progress to swelling, anaphylaxis, and even death. Peanuts, seafood and tree nuts are the most likely to progress to anaphylaxis.
Food poisoning can cause violent gastrointestinal symptoms, but would not include the other more characteristic “allergic” reactions, such as hives or wheezing. In addition, others who ate the food would most likely also get ill, and the same food at another time would not generate a reaction. However, food poisoning can be serious; so do seek medical attention.
Avoidance is the only way to prevent a food-related reaction, since there is no medication or vaccine currently available for prevention. For ultra-sensitive individuals, avoidance requires vigilant reading of food labels, with a preference for fresh ingredients rather than prepared/processed foods.
Even minute amounts of the offending allergen can elicit severe reactions in hypersensitive individuals. For example, a cookie factory inadvertently can contaminate cookies with peanut butter that are labeled as without peanut butter. One bite could send a hypersensitive individual into anaphylaxis. Vigilance is also required when eating out, as ingredients not mentioned in the menu may be used in the food’s preparation. It is always best to specify, so ask before ordering and let the restaurant know you have a severe allergy. In prepared foods, the allergen may actually be an additive or preservative. If you can tolerate the food at home, or in fresh form, but not when pre-packaged or in a restaurant, this may be why.
Reactions to food may be linked to other allergies from which the individual suffers. People allergic to ragweed, for example, may also react to melons. In addition, food labels can be confusing. For example, egg whites may be listed as “albumin,” or wheat as “gluten.” People allergic to eggs are usually advised to avoid the flu vaccine, as it is prepared with a substance present in egg whites. Also, since dyes are sometimes used in the preparation of certain medications, check with your doctor if you are allergic to a dye/food coloring before taking any over-the-counter preparation for the first time, or when seeing a new physician and receiving a prescription.
If you have a food allergy, discuss with your physician the need to carry an emergency epinephrine kit or wear “medic alert” identification. (See Diagnosis for discussion of the “elimination” diet.
7. Latex Allergy
An allergy to latex has been steadily on the increase. Latex is the processed form of the milky sap derived from natural rubber trees. As with other allergies, the possibility of an allergic reaction increases with each exposure to the protein. Therefore, those most at risk are those with frequent exposure to latex. While a synthetic latex exists, this does not generate an allergic reaction, since it does not contain the allergenic protein.
The use of latex has increased dramatically with the use of latex gloves as a barrier against the transmission of infectious diseases. Those most at risk are health care workers, including dentists, technicians, housekeeping personnel and food service workers. However, law enforcement personnel, firefighters, EMTs, and workers in the manufacturing plants for latex products also are at risk. Individuals with multiple allergies, and those with frequent, early medical intervention, such as with spina bifida, are also at increased susceptibility.
Avoidance of the offending allergen is critical. However, it may be harder than you think. Latex is not just in gloves but in thousands of medical products such as IV tubing, catheters and bandages. Outside the medical arena, latex is used in tires, condoms, shoe soles, clothing (waistbands), erasers, rubber bands, swimming goggles, toys, and pacifiers. Some products, like balloons, can substitute Mylar for latex, but for many products no substitute is available.
Early symptoms include skin reactions:
- Rashes, hives and flushing
- Itching, congestion, eye irritation, wheezing, asthma and progression into anaphylaxis.
Sensitive individuals may experience itching in the mouth after a dental exam, for example. Those allergic to the following foods may also be sensitive to latex: avocados, bananas, potatoes, tomatoes, hazelnuts, chestnuts, kiwi and papayas.
While direct skin contact is a problem, the allergen also can be inhaled. This primarily occurs when gloves are taken off and the protein, which has combined with the powder inside the glove becomes airborne. It is also important to avoid the use of oil-based creams and lotions when using latex gloves, as glove deterioration can occur and allow more protein particles to escape.
If you suspect you have developed a latex allergy, avoid any contact with latex until a diagnosis can be confirmed. Let others know of your allergy. Even food served by cafeteria workers wearing latex gloves can create a reaction. Discuss with your physician the need for an emergency epinephrine kit and the wearing of a medic alert bracelet.

